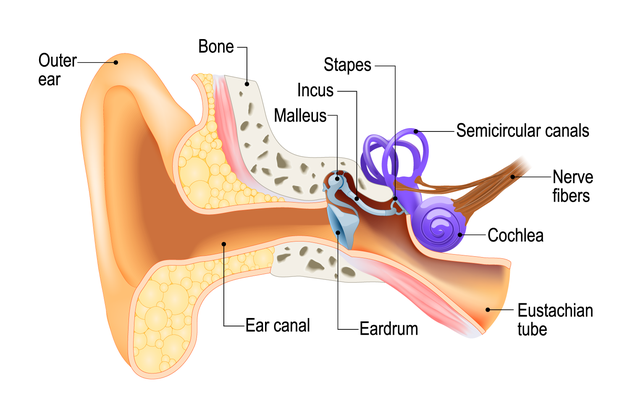
OTOSCLEROSIS
Definition: Otosclerosis is a hereditary localized disease originating from the otic capsule in which mature lamellar bone is removed by osteoclasts and replaced by woven bone of greater thickness, cellularity and vascularity. There is commonly a fixation in the Incudo-stapedial joint which fails or reduces the sound conduction resulting in deafness.
Aetiology:
- Age: Common in the second and third decade.
- Race: Common in whites than blacks.
- Sex: Male to female ratio is 3:2.
- Pregnancy: Otosclerosis commonly increases post pregnancy. 1 in 24 pregnant females develop the disease.
- Other causative theories.
- Theory of metabolic disorder.
- Infective theory.
- Traumatic theory.
- Theory of vascular disease.
Types of Otosclerosis:
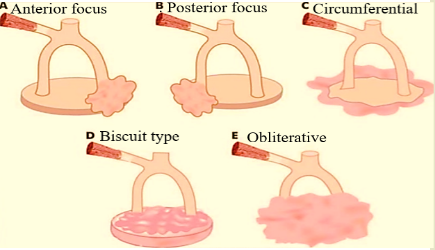
- Stapedial Otosclerosis: Occurs due to fixation of the stapes footplate. It is the most common variety. Here, otosclerosis starts just in front of oval window at “Fistula ante fenestra.” This is the site of anterior focus. Lesion may start behind oval window, called posterior focus, around margin of stapes footplate (circumferential), in the footplate but the annular ligament is free (biscuit type), it may completely obliterate oval window (obliterative type).
- Cochlear Otosclerosis: Cochlear otosclerosis involves the round window or other areas in the otic capsule, and cause sensorineural hearing loss due to liberation of toxic materials into the inner ear fluid.
- Histologic Otosclerosis: This type of otosclerosis remains asymptomatic and causes neither conductive nor sensorineural hearing loss.
- Deafness: The deafness is usually bilateral occurring between the third and fifth decade. Audiometry shows a typical conductive hearing loss at 2000 Hz called Carhart notch. An Impedance audiometry confirms the ossicular fixation.
- Tinnitus: It is an indication of sensorineural hearing loss which is seen in patients having this disease since a long period.
- Vertigo: These attacks are usually transient as a result of toxic enzymes.
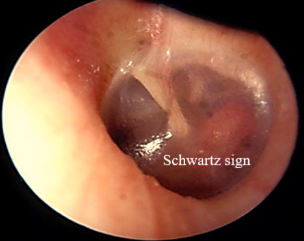
- Occasionally, a reddish hue may be seen on the promontory through the tympanic membrane (Schwartz sign). This is indicative of active focus with increased vascularity.
Investigation:
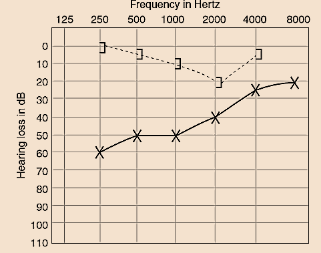
1. Pure tone audiometry–
- Loss of air conduction, more for lower frequencies.
- Bone conduction is normal. In few cases, there is a dip in bone conduction curve, maximum at 2000 Hz and is called Carhart’s notch (5 dB at 500 Hz, 10 dB at 1000 Hz, 15 dB at 2000 Hz and 5 dB at 4000 Hz). Carhart’s notch disappears after successful stapedotomy.
- Mixed hearing loss may also be present. There is loss in bone conduction with air-bone gap.
2. Speech audiometry shows normal discrimination score except in those with cochlear involvement.
3. Tympanometry is normal in early cases but later shows Ad type of curve (ossicular stiffness).
4. Stapedial reflex becomes absent when stapes is fixed.
Differential diagnosis:
1. Medical line of treatment: Oral sodium fluoride therapy can be given 50 mg daily for a period of 6 months to 1 year, depending on the tolerance level of the patient. However,this therapy is usually for medically unfit patients and results are unreliable. 2. Surgical treatment: A. Conventional Stapedotomy –
- Serous otitis media.
- Adhesive otitis media.
- Tympanosclerosis.
- Attic fixation of head of malleus.
- Ossicular discontinuity.
- Congenital stapes fixation.
1. Medical line of treatment: Oral sodium fluoride therapy can be given 50 mg daily for a period of 6 months to 1 year, depending on the tolerance level of the patient. However,this therapy is usually for medically unfit patients and results are unreliable. 2. Surgical treatment: A. Conventional Stapedotomy –
-
- Rosen’s endomeatal incision is given from 12 O’ clock to 6 O’ clock position 6 mm to 8 mm away from the annulus.
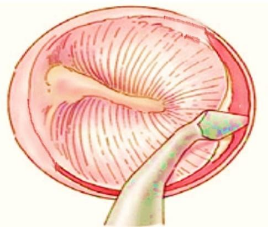
- Tympanomeatal flap is raised and annulus is elevated to enter the middle ear.
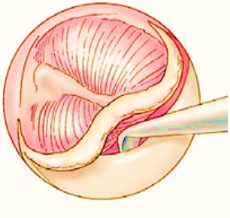
- Middle ear is inspected. Chorda tympani nerve elevated carefully
- Posterosuperior quadrant is curetted, care taken not to damage the Chordae tympani nerve.
- Exposure till the pyramidal process is done.
- Incudostapedial joint is visualized.
- Stapes fixation is confirmed by testing ossicular mobility.
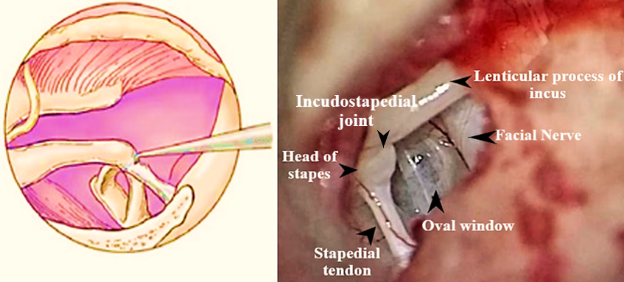
- The stapedial tendon is cut near its origin from pyramidal process.
- The posterior crus is better seen thereafter.
- Mucosa between incudo-stadedial joint is dissected and the incudo-stapedial joint is dislocated.
- Stapes suprastructure is fractured either by pick or microdebridor drill.

- Mucosa over the stapes footplate is gently teased off with a sharp pick.
- Footplate is then thinned using microdebrider skeeter burr.

- Small controlled fenestra (opening) is made on the fixed stapes footplate. Initially 0.3 mm Fisch perforator is used. Gradually, fenestra is widened with 0.4mm or 0.6 mm perforator or microdrill.
- Distance between the undersurface of footplate and lateral surface of incus is measured using house measuring rod and piston is cut accordingly by placing it on jig measuring scale.
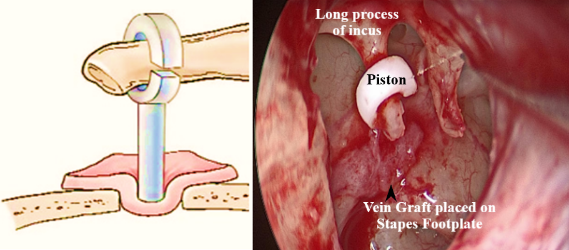
- Vein graft is placed to cover the opening of the footplate.
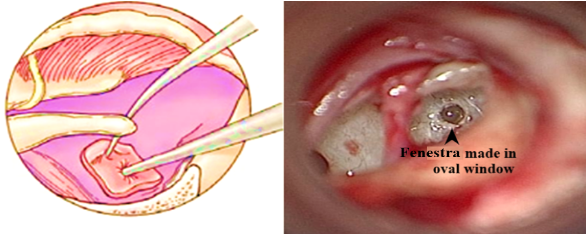
- Piston is first placed on the fenestra, then align it with the long process of incus.

- Crimping of piston done.
- Ossicular chain mobility is checked.
- Tympanomeatal flap is replaced.
Reverse Stapedotomy-
- Here the stapedial tendon and the incudo-stapedial joint is preserved while making fenestration in stapes footplate.
- Piston is first placed on the fenestra, then aligned with the long process of incus.
- Crimping of piston done.
- After this, the stapedial tendon is cut near its origin from pyramidal process.
- The posterior crus is better seen thereafter.
- Mucosa between incudo-stapedial joint is cleared and the joint is dislodged.
- Stapes suprastructure is fractured.
- Ossicular chain mobility is checked.
- Tympanomeatal flap is replaced.
This procedure is done to decrease the incidence of accidental footplate subluxation.
C. LASERS (Potassium titanyl phosphate KTP, Argon, CO2) are used to make precise fenestra with a minimal risk of acoustic or mechanical trauma. It is especially useful in conditions like floating footplate.
We Are Always Ready to Help You.
Book An Appointment

