
FNAC IN ENT
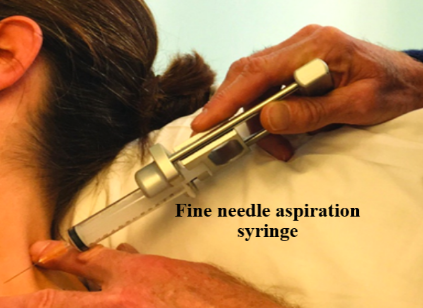
Preparation of the patient:
- No aspirin or non-steroidal anti-inflammatory medications (e.g., ibuprofen, naproxen) for one week before the procedure.
- Routine blood tests (including clotting profile) must be completed two weeks before the biopsy.
- Stoppage of anticoagulants (blood thinners).
- Antibiotic prophylaxis may be instituted.
Before the procedure, vital signs like pulse, blood pressure, temperature etc should be measured. Then, depending on the nature of the biopsy, an intravenous line may be placed. Very anxious patients can be sedated through this line, or oral medication (Valium) may be prescribed.
Procedure:
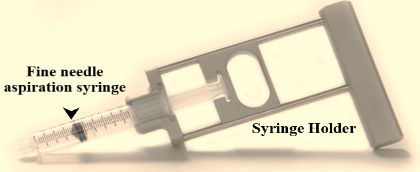
The skin above the area to be biopsied is swabbed with an antiseptic solution and draped with sterile surgical towels. The skin, underlying fat, and muscle may be numbed with a local anesthetic, although this is often not necessary with superficial masses. After locating the mass for biopsy, using x-rays or palpation, a special needle of very fine diameter (23–25 gauge (0.52 to 0.64 mm outer diameter)) is passed into the mass. The needle may be inserted and withdrawn several times. There are many reasons for this:
- One needle may be used as a guide, with the other needles placed along it to achieve a more precise position.
- Sometimes, several passes may be needed to obtain enough cells for the intricate tests which the cytopathologists perform.
After the needles are placed into the mass, aspirate is removed and then spread on a glass slide. Finally, the cells are stained and visualized under microscope. The patient’s vital signs are taken again, and the patient is removed to an observation area for three to five hours.
FNAC can also be done under ultrasound and CT scan guidance.
Most common indications are:
1) Salivary gland swellings:
FNAC of the salivary glands is helpful because it often differentiates benign from malignant swellings. It thus changes the management.
Common salivary gland swellings are:
a) Pleomorphic adenoma.
b) Acinic cell carcinoma.
c) Adenoid cystic carcinoma.
Findings:
A normal FNAC of the salivary gland would show:
a) Acinar cells.
b) Ductal epithelial cells.
2) Lymph nodes:
Advantages:
a) Does not require anesthesia.
b) False positive result is rare.
c) No scar left behind.
d) Often the site of primary lesion can be diagnosed on FNAC.
e) Avoids surgery if not indicated.
Common lymph node conditions:
a) Tuberculous lymphadenitis.
b) Chronic inflammatory lymphadenitis.
c) Secondary metastatic lymph nodes.
d) Malignant lymphoma.
e) Burkitt’s lymphoma.
f) Hodgkin’s lymphoma.
g) Non Hodgkins lymphoma.
3) Thyroid swellings:
FNAC of thyroid has been established as an important diagnostic test for evaluation of benign and malignant thyroid swellings.
Major indications:
a) Diagnosis of diffuse non-toxic goiters.
b) Confirmation of clinically obvious thyroid malignancy.
c) Diagnosis of solitary thyroid nodule.
d) Acute suppurative thyroiditis.
e) Follicular neoplasm.
f) Papillary carcinoma of thyroid.
g) Medullary carcinoma.
h) Cyst / hemorrhage in thyroid gland.
i) Medullary carcinoma.
4) FNAC can also be done for oral, oropharyngeal, buccal, and tongue lesions.
- Hemorrhage.
- Vasovagal shock.
- Hematoma.
- Tracheo-oesophageal puncture.
- Damage to major blood vessels in the neck.
We Are Always Ready to Help You.
Book An Appointment

